HEAT EXHAUSTION
So that you don't tip over into heat stroke, this column is from Scouting Magazine.
Now let’s make a distinction: Heat exhaustion is different from heat stroke. This deals with the former, which can lead to the latter — but they are not the same thing. Heat stroke is a serious condition that can be fatal and demands urgent hospital care. (Recovery requires immediate full-body cooling to avoid permanent brain injury or death.)
Heat exhaustion, while serious, can be field-treated in most cases if you know what you’re doing.
Heat exhaustion is the body’s way of telling you that it's water- and salt-depleted, typically because of excessive perspiration without proper replenishment. There are numerous signs of the condition: profuse sweating (as the body tries to cool itself), dizziness, fatigue and muscle cramps. Other signs might be less obvious: general confusion, very dark yellow (or even brownish) urine, nausea and a rapid heart rate.
The first step in treating heat exhaustion is to stop, sit and cool down. Next, move to a cool(er) place. If you’re near a swimming hole, go for it. If not, move to a shady spot (try a north-facing slope).
Once you cease activity, rehydrate slowly while removing tight-fitting clothing. Water is a good choice. But because heat exhaustion might also be caused by mineral depletion, electrolyte-enhanced sports drinks are also effective. If a banana is available, eat one for added mineral replenishment. Salt tablets can also be dissolved in water, but don’t overdo it … you’re trying to rehydrate, not dehydrate. Rehydrate with a mouthful of liquid at a time. This should eventually lead to urination, a sign that the kidneys are functioning normally and the body is no longer fluid-depleted.
There are additional ways to treat heat exhaustion. Full-body immersion in cool water is ideal. If you have water to spare, cool the victim’s skin with dampened T-shirts. Also, fanning speeds up the skin-cooling effects of sweating. Use a map, book, magazine or hat. A few people fanning the overheated hiker can be helpful.
Recovery times vary for heat exhaustion. Don’t expect someone to take off down the trail after swallowing some Gatorade. Activity should be kept to a minimum. If you need to hike out, wait until it’s cooler and then take your time.Untreated Heat Exhaustion can rapidly turn into Heat Stroke. The factors that cause, raise the risk factor or can exacerbate heat exhaustion are the same for heat stroke. The main sign that someone is going into heat stroke when hiking is that their body temperature can reach 104 - 105 F and beyond at which point the hikers may exhibit personality changes, confusion and even go into a coma.
HEAT STROKE
Heat stroke is much more dangerous than heat exhaustion, and requires swift action, because the body’s core temperature has reach a life-threatening 105 degrees or higher. The main symptoms to look for with heat stroke are:
- Skin red, hot to the touch
- Irritability
- confusion or unconsciousness
- Feeling dizzy or lightheaded
- Rapid heartbeat
- Rapid and shallow breathing
- Elevated or lowered blood pressure
- Cessation of sweating
- Headache
- Nausea
- Fainting (Often the first sign in older adults)
With heat stroke it is imperative that you get the victim to medical help immediately. The victim’s temperature needs to be lowered quickly. If you are in an area that is too far for swift medical help, you must move the individual to shade, loosen tight clothing, and have him drink small amounts of cool water. Pour water on them and increase cooling by fanning. If traveling in a group of three or more, send one for help. Do not leave the victim alone. Carefully monitor the victim to prevent a relapse.
If for any reason you or your trail partner is not recovering, don't hesitate to call 911.
More good tips:
For dog walkers
Care: How To Prevent Your Dog From Overheating On The Hiking Trail
<http://www.care2.com/causes/how-to-prevent-your-dog-from-overheating-on-the-hiking-trail.html>
Runner's World: How to avoid overheating on the run
<http://www.runnersworld.com/fuel-school/how-to-avoid-overheating-on-the-run>
For horses:
Equisearch: How to keep your horse cool on the trail
<https://www.equisearch.com/resources/eqcool396>
For hikers and all trail users:
Scouting: How to prevent and overcome heat exhaustion
https://scoutingmagazine.org/2015/04/how-to-survive-heat-exhaustion/
For bikers:
Active: Avoid Heat Stress When You Ride
<http://www.active.com/cycling/articles/avoid-heat-stress-when-you-ride-with-these-tips>
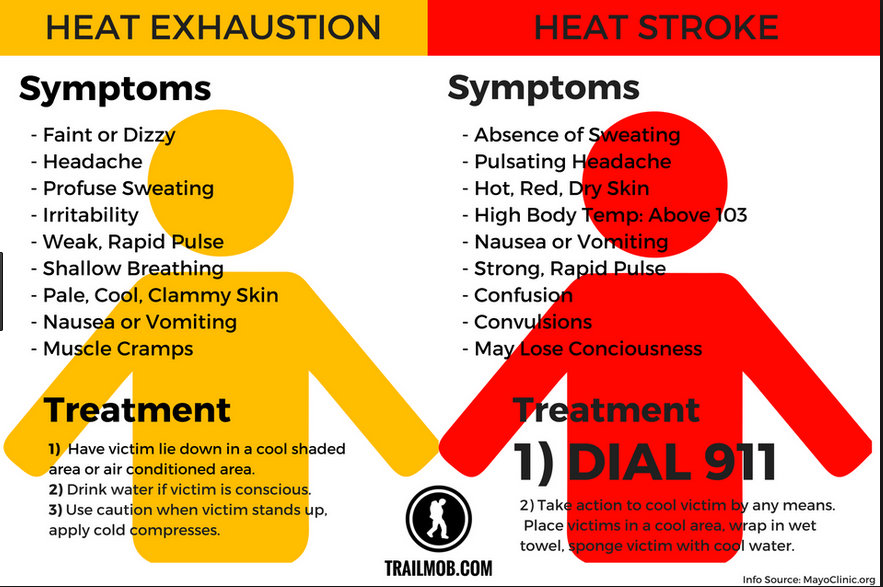
Poster from the Mayo Clinic.
 RSS Feed
RSS Feed